Racial/ethnic disparities in gallbladder cancer receipt of treatments
Introduction
Although rare, gallbladder cancer is the fifth most common cancer involving gastrointestinal tract and the most common cancer of the biliary tract accounting for 80–95% of biliary tract cancers (1,2). Resection is the only potentially curative treatment in early-stage tumors. Due to the asymptomatic nature in the early stages, this cancer is usually detected in an advanced non-curative stage with a dismal prognosis (2). Several efforts have been made to raise awareness for earlier detection of this lethal disease (3). Despite those efforts, the number of incidental gallbladder cancer after cholecystectomy for cholelithiasis has remained fairly stable in the past two decades (4). Beside early detection, improved imaging modalities, aggressive surgical approach, and adjuvant therapy in the last decade have improved gallbladder cancer survival significantly (5,6). However overall median survival is still dismal at 4 months (7).
Racial/ethnic disparities in survival exist. Though overall survival has improved in almost all races/ethnicities, Hispanics and blacks have shown no survival improvements over the past decade (8). Despite improvements in gallbladder cancer management, it is not clear whether racial/ethnic disparities in stage at diagnosis and receipt of treatments exist that could be the source of survival disparities and the areas for future research. This current study used a large, ethnically diverse population-based cancer registry to evaluate race/ethnicity-specific trends in the stage of disease and receipt of treatments among adult gallbladder cancer patients in the US.
Methods
Data source
Surveillance, Epidemiology, and End Results (SEER) population-based cancer registry (version November 2015) was used for the analysis (9). We analyzed data from 18 population-based cancer registries including Atlanta, Connecticut, Detroit, Hawaii, Iowa, New Mexico, San Francisco-Oakland, Seattle-Puget Sound, Utah, Los Angeles, San Jose and Monterrey, Rural Georgia, the Alaska Native Tumor Registry, Greater California, Kentucky, Louisiana, New Jersey, and Greater Georgia, which cover approximately 28% of the US population.
Study cohort
All patients aged 20 years or older newly diagnosed with gallbladder cancer [corresponding to International Classification of Diseases for Oncology, Third Edition (10), code C23.9] with the following histologic subtypes: adenocarcinoma (codes 814.0-814.7); papillary carcinoma or papillary adenocarcinoma (codes 805.0-805.2 and 826.0-826.3); adenosquamous carcinoma (codes 856.0-856.2 and 857.0); or other cancers (849.0 signet ring, 804.0-804.6 small cell, 801.0-801.5 carcinoma not otherwise specified, or 802.0-802.2 undifferentiated carcinoma) from 2000 to 2013 were recruited. Exclusion criteria included patients with any other histologic subtypes; patients with unknown age; patients with unknown race/ethnicity; and patients in whom the diagnosis was found on an autopsy or listed only on the death certificate.
Data abstraction and variables
Demographic variables (age at diagnosis, sex, race/ethnicity), tumor characteristics (historic stage) and treatments [radiation therapy, surgery, and lymph node (LN) clearance] were obtained from the registry database. We defined race/ethnicity as self-reported constructs including Hispanics (regardless of race), non-Hispanic black (blacks), non-Hispanic white (whites), non-Hispanic Asian and Pacific Islander (Asians). Historic stage was categorized into early and advanced stage. According to the American Joint Committee on Cancer (AJCC) TNM staging classification (11), early stage is defined as patients with T1, T2 or T3 and M0 disease, which are amenable for curative surgery. Patients with carcinoma in situ were excluded. Type of treatments was determined using SEER site-specific surgery of primary site codes and radiation therapy codes. Curative surgery was defined based on data availability in SEER as simple resection and radical resection. Simple resection was defined as cholecystectomy with or without LN dissection. Radical resection was defined as cholecystectomy with a resection in continuity with other organs with or without LN dissection. Since extensive lymphadenectomy correlates with longer survival even in node-negative patients (12), number of LNs removed was abstracted in patients who underwent curative surgery. Optimal LN clearance was defined as more than four LNs removed according to a previous study (12).
Statistical analysis
Demographic and clinical data among different racial/ethnic groups were presented as frequency (N) and proportion (%) for categorical variables, or mean and standard deviation (SD) for continuous variables. The χ2 test was used for comparing categorical variables and analysis of variance was used for comparing continuous variables. Differences in gallbladder cancer stage at presentation, gallbladder cancer treatment modalities and number of LN examined among racial/ethnic groups were evaluated using multivariate logistic regression models. All models were adjusted for age, sex, year of diagnosis, and stage of disease. Subgroup analyses were performed to analyze the trends in stage at diagnosis and treatment disparities among races/ethnicities by dividing into 2-time periods: 2000–2006 and 2007–2013. A 2-sided P value of ≤0.05 was considered significant. All analyses were conducted using IBM SPSS Statistics (version 21.0. Armonk, NY, USA). Review by the institutional review board was not required for this study as the SEER database is publicly available without individually identifiable private information.
Results
Baseline characteristics
A total of 7,507 patients with newly diagnosed gallbladder cancer from 2000 to 2013 were included in this study. The majority of gallbladder cancer patients were female (71.6%) with the mean age of 69.6±12.9 years. Compared with whites, blacks had a significantly younger age at diagnosis (65.5 vs. 71.8 years, P<0.001). Curative surgery, defined as simple resection and radical resection, was performed in 5,429 patients out of 6,210 patients with early-stage gallbladder cancer (87.4%). Radiation was performed in 1,084 patients (14.4%). Optimal LN dissection was performed in 648 patients of 5,429 patients who underwent curative surgery (11.9%) (Table 1).
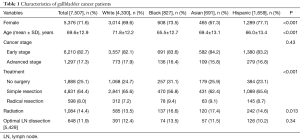
Full table
Disparities in stage of disease at presentation
As we categorized stage at diagnosis into early and advanced stage based on AJCC classification, there were no racial/ethnic disparities in stage of disease at presentation. After stratifying patients into 2-time periods (2000 to 2006 and 2007 to 2013), we found no racial/ethnic disparities in stage at diagnosis in both time periods (Table 2).
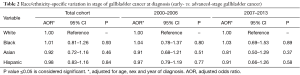

Full table
Disparities in gallbladder cancer treatments
Compared with whites, blacks were significantly less likely to receive curative surgery [adjusted odds ratio (AOR) 0.67, 95% CI: 0.56–0.80; P<0.001] whereas Hispanics and Asians had no differences in receiving curative surgery compared to whites (Table 3). As we stratified patients into 2-time periods, no significant differences in receiving surgery were found among races/ethnicities from 2000 to 2006 but racial/ethnic disparities existed between 2007 and 2013 as blacks were less likely to receive curative surgery compared to Whites (AOR 0.57, 95% CI: 0.45–0.71; P<0.001) (Table 3).
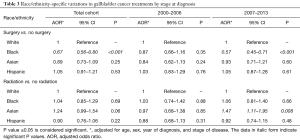
Full table
With regard to radiation therapy, there were no racial/ethnic disparities in receiving radiation therapy among races/ethnicities. However, after stratification into 2-time periods, Asians were significantly more likely to receive radiation compared to whites (AOR 1.47, 95% CI: 1.11–1.95; P=0.008) between 2007 and 2013 (Table 3). There were no racial/ethnic disparities in radiation therapy between 2000 and 2006.
Among patients undergoing curative surgery, Hispanics were significantly less likely to receive optimal LN clearance compared to whites (AOR 0.59, 95% CI: 0.47–0.74; P<0.001) (Table 4) and this disparity of receiving optimal LN clearance has got worse in Hispanics over time when comparing between 2-time periods.
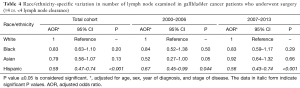
Full table
Discussion
Our study observed no racial/ethnic disparities in gallbladder cancer stage at presentation. However, significant racial/ethnic disparities in gallbladder cancer treatments were observed. Compared with whites, blacks, and Hispanics were less likely to receive curative surgery, and optimal LN clearance, respectively and Asians were more likely to receive radiation than whites. Moreover, these disparities seem to be more pronounced over time.
A previous study demonstrated significant racial/ethnic disparities in survival improvements of gallbladder cancer (8). In the past decade, overall survival has improved in all races/ethnicities except Hispanics and blacks. Since survival depends a lot on an early diagnosis, no studies to date have addressed whether there are racial/ethnic disparities in stage at diagnosis, which could be the source of survival disparities among races/ethnicities. These issues have been explored in other cancers. A previous study found racial/ethnic disparities in stage at diagnosis of hepatocellular carcinoma patients as blacks had significantly more advanced stage at diagnosis than whites (13). Racial disparities in stage at diagnosis were also found in patients with colorectal cancer where blacks were more likely present at advanced stage with a higher risk of mortality compared to whites and this gap has widened over time (14,15). However, our study observed no racial/ethnic disparities in gallbladder cancer stage at diagnosis. The exact reason is unclear, however we could imply that several raising awareness programs have been equally implemented among races/ethnicities in the US.
Another potential source of disparities in the improvements of survival among races/ethnicities is disparities in treatments received. A resection provides the only chance for a cure for early-stage gallbladder cancer (2). Optimal LN dissection has also been shown to improve survival in all stages of gallbladder cancer even in node-negative patients (12). Compared with whites, our study found that blacks, and Hispanics were less likely to receive curative surgery and optimal LN dissection, respectively and these disparities are more pronounced over time. These findings are consistent with a lack of survival improvements in blacks and Hispanics (8). Not only gallbladder cancer, blacks and Hispanics were found to be less likely to receive curative treatments (tumor resection and liver transplantation) in patients with hepatocellular carcinoma (13). Blacks were found to be less likely to receive treatments in all stages of colorectal cancer (14,16). Another study demonstrated that blacks were less likely to receive pancreatic cancer surgery compared to whites with no significant changes in the trends from 1988 to 2009 (17). The reasons for the treatment disparities among races/ethnicities and its increment over time in our study are unknown, however issues of socioeconomic and insurance inequalities could play a role. Both factors can affect health care access and are associated with poor cancer outcomes (18,19). Blacks and Hispanics have 1.5 to 3 times higher uninsured rates than whites, which could cause limited access to health care (20,21). One study also found that blacks were less likely to be recommended for surgery and were more likely to refuse surgery (17).
Our study has several strengths. First, SEER is one of the largest cancer databases in the US, which allows for recruitment of a large sample size given the rarity of gallbladder cancer. Second, regional variations in health care delivery, which commonly limit in smaller studies, were minimized because samples were taken broadly cross the US, which provides the generalizability of our results with a national perspective. Third, consistent case definitions with respect to race/ethnicity, tumor stage, and treatments ensured accuracy of our analyses.
However, our study has some limitations that should be acknowledged. First, due to the limitations of the SEER database, we did not have information regarding patients’ comorbidities, patients’ functional status, liver function, and severity of ascites, vascular encasement or occlusion from tumors that could affect treatment eligibility. Second, the SEER treatment data is limited to the first course of treatment; does not include a complete therapeutic course. However, this study of racial/ethnic disparities in gallbladder cancer stage at diagnosis and gallbladder cancer treatment will definitely improve understanding of gallbladder cancer survival disparities in the US.
In summary, no racial/ethnic disparities were observed in gallbladder cancer stage at diagnosis. However, blacks and Hispanics were found to significantly have lower rates of receiving gallbladder cancer treatments. These findings are consistent with the previous study, which demonstrated a lack of gallbladder cancer survival improvements over time in these two groups. The disparity in survival among races/ethnicities appears to have been affected more strongly by treatments than disease stage at diagnosis. Findings from this study could help profile and target patients with the greatest disparities in gallbladder cancer health outcomes. Further researches are needed to address treatment disparities in blacks and Hispanics.
Acknowledgements
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Ethical Statement: Ethical approval by the institutional review board was not required for this study as the SEER database is publicly available without individually identifiable private information. Informed consent was not required for this study as the SEER database contains fully anonymised data.
References
- Hundal R, Shaffer EA. Gallbladder cancer: epidemiology and outcome. Clin Epidemiol 2014;6:99-109. [PubMed]
- Rakic M, Patrlj L, Kopljar M, et al. Gallbladder cancer. Hepatobiliary Surg Nutr 2014;3:221-6. [PubMed]
- February is National Gallbladder and Bile Duct Cancer Awareness Month. Jacksonville Progress. 2017. Available online: http://www.jacksonvilleprogress.com/news/february-is-national-gallbladder-and-bile-duct-cancer-awareness-month/article_777c3c06-ed53-11e6-bc9d-a3d4dff472d2.html. Accessed June 24 2017.
- Dorobisz T, Dorobisz K, Chabowski M, et al. Incidental gallbladder cancer after cholecystectomy: 1990 to 2014. Onco Targets Ther 2016;9:4913-6. [Crossref] [PubMed]
- Dixon E, Vollmer CM Jr, Sahajpal A, et al. An aggressive surgical approach leads to improved survival in patients with gallbladder cancer: a 12-year study at a North American Center. Ann Surg 2005;241:385-94. [Crossref] [PubMed]
- Andren-Sandberg A. Diagnosis and management of gallbladder cancer. N Am J Med Sci 2012;4:293-9. [Crossref] [PubMed]
- Kiran RP, Pokala N, Dudrick SJ. Incidence pattern and survival for gallbladder cancer over three decades--an analysis of 10301 patients. Ann Surg Oncol 2007;14:827-32. [Crossref] [PubMed]
- Jaruvongvanich V, Yang J, Peeraphatdit T, et al. The incidence rates and survival of gallbladder cancer in the USA. Eur J Cancer Prev 2017. [Epub ahead of print]. [Crossref] [PubMed]
- Surveillance, Epidemiology, and End Results (SEER) Program () SEER*Stat Database: Incidence - SEER 18 Regs Research Data + Hurricane Katrina Impacted Louisiana Cases, Nov 2015 Sub (1973–2013 varying) - Linked To County Attributes - Total U.S., 1969–2014 Counties, National Cancer Institute, DCCPS, Surveillance Research Program, Surveillance Systems Branch, released April 2016, based on the November 2015 submission.www.seer.cancer.gov
- World Health Organization. International Classification of Diseases for Oncology. 3rd ed. Geneva: WHO.
- Edge SB, Compton CC. The American Joint Committee on Cancer: the 7th edition of the AJCC cancer staging manual and the future of TNM. Ann Surg Oncol 2010;17:1471-4.
- Tran TB, Nissen NN. Surgery for gallbladder cancer in the US: a need for greater lymph node clearance. J Gastrointest Oncol 2015;6:452-8. [PubMed]
- Ha J, Yan M, Aguilar M, et al. Race/Ethnicity-specific Disparities in Hepatocellular Carcinoma Stage at Diagnosis and its Impact on Receipt of Curative Therapies. J Clin Gastroenterol 2016;50:423-30. [PubMed]
- Robbins AS, Siegel RL, Jemal A. Racial disparities in stage-specific colorectal cancer mortality rates from 1985 to 2008. J Clin Oncol 2012;30:401-5. [Crossref] [PubMed]
- Tawk R, Abner A, Ashford A, et al. Differences in Colorectal Cancer Outcomes by Race and Insurance. Int J Environ Res Public Health 2015;13:ijerph13010048.
- Lai Y, Wang C, Civan JM, et al. Effects of Cancer Stage and Treatment Differences on Racial Disparities in Survival From Colon Cancer: A United States Population-Based Study. Gastroenterology 2016;150:1135-46. [Crossref] [PubMed]
- Shah A, Chao KS, Ostbye T, et al. Trends in racial disparities in pancreatic cancer surgery. J Gastrointest Surg 2013;17:1897-906. [Crossref] [PubMed]
- Niu X, Roche LM, Pawlish KS, et al. Cancer survival disparities by health insurance status. Cancer Med 2013;2:403-11. [Crossref] [PubMed]
- Cella DF, Orav EJ, Kornblith AB, et al. Socioeconomic status and cancer survival. J Clin Oncol 1991;9:1500-9. [Crossref] [PubMed]
- Riley P, Hayes SL, Ryan J. Closing the Equity Gap in Health Care for Black Americans. To the Point, The Commonwealth Fund, July 15, 2016.
- Doty MM, Beutel S, Rasmussen PW, et al. Latinos Have Made Coverage Gains but Millions Are Still Uninsured. The Commonwealth Fund Blog, April 27, 2015.


